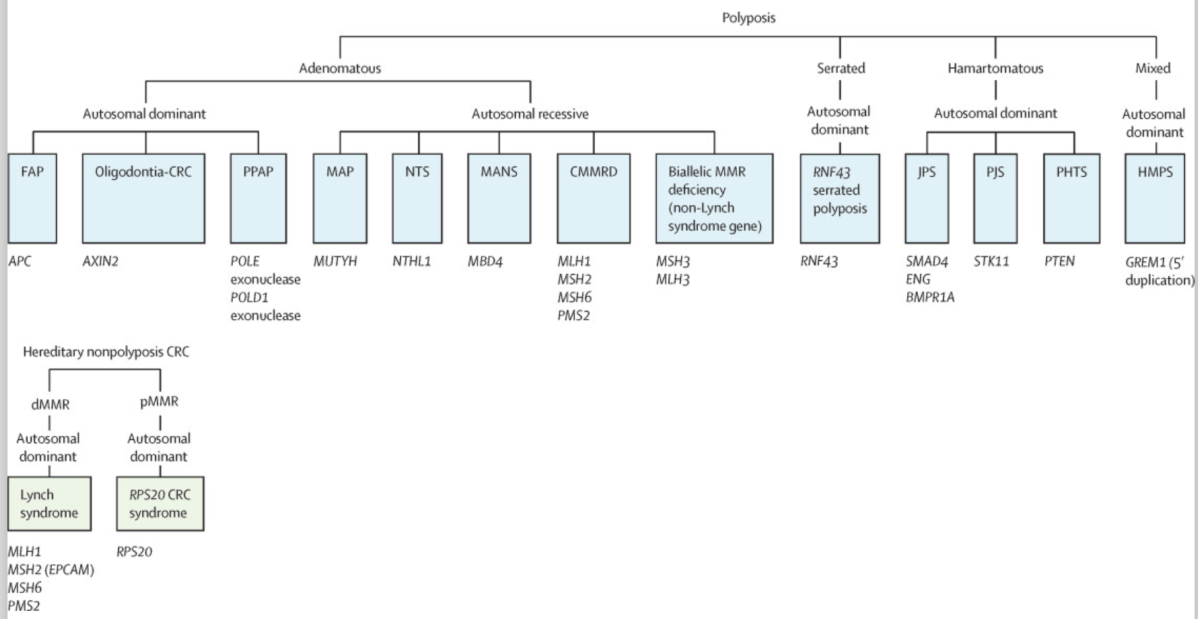
Lynch syndrome is caused by an inherited mutation in one of these genes:
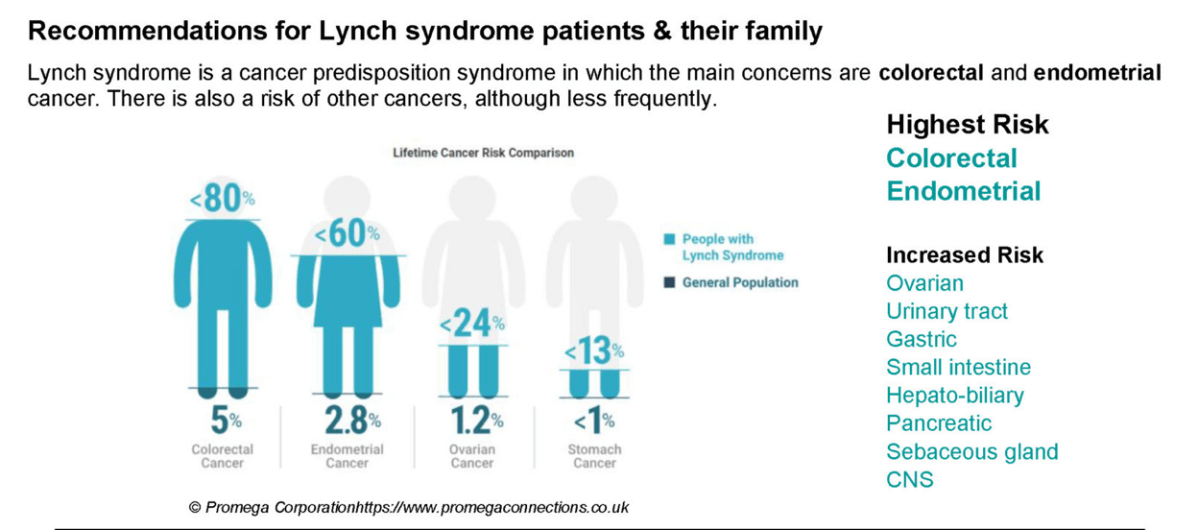
People with Lynch syndrome have an increased risk for colorectal, endometrial and other cancers. The cancer risk varies by gene mutation, therefore it is important for people with Lynch syndrome to know which gene mutation they have.
In the past, the risk-management guidelines were the same for people with an inherited mutation in any of the Lynch syndrome genes. As more research has shown different cancer risks for each gene, experts have started to separate the risks and medical options for each individual mutation. Despite these differences, some references discuss Lynch syndrome as though inherited mutations in these genes carry the same risks.
If you have been told that you have Lynch syndrome, it is important to know which gene has a mutation, so that you can make informed decisions about your medical care.
In the past, Lynch syndrome was also referred to as “hereditary nonpolyposis colorectal cancer” (HNPCC). This term has fallen out of favour because mutations in these genes also increase the risk for other cancers besides colorectal cancer.