Identification and development of novel colorectal cancer biomarkers via state-of-the-art liquid biopsy approaches.
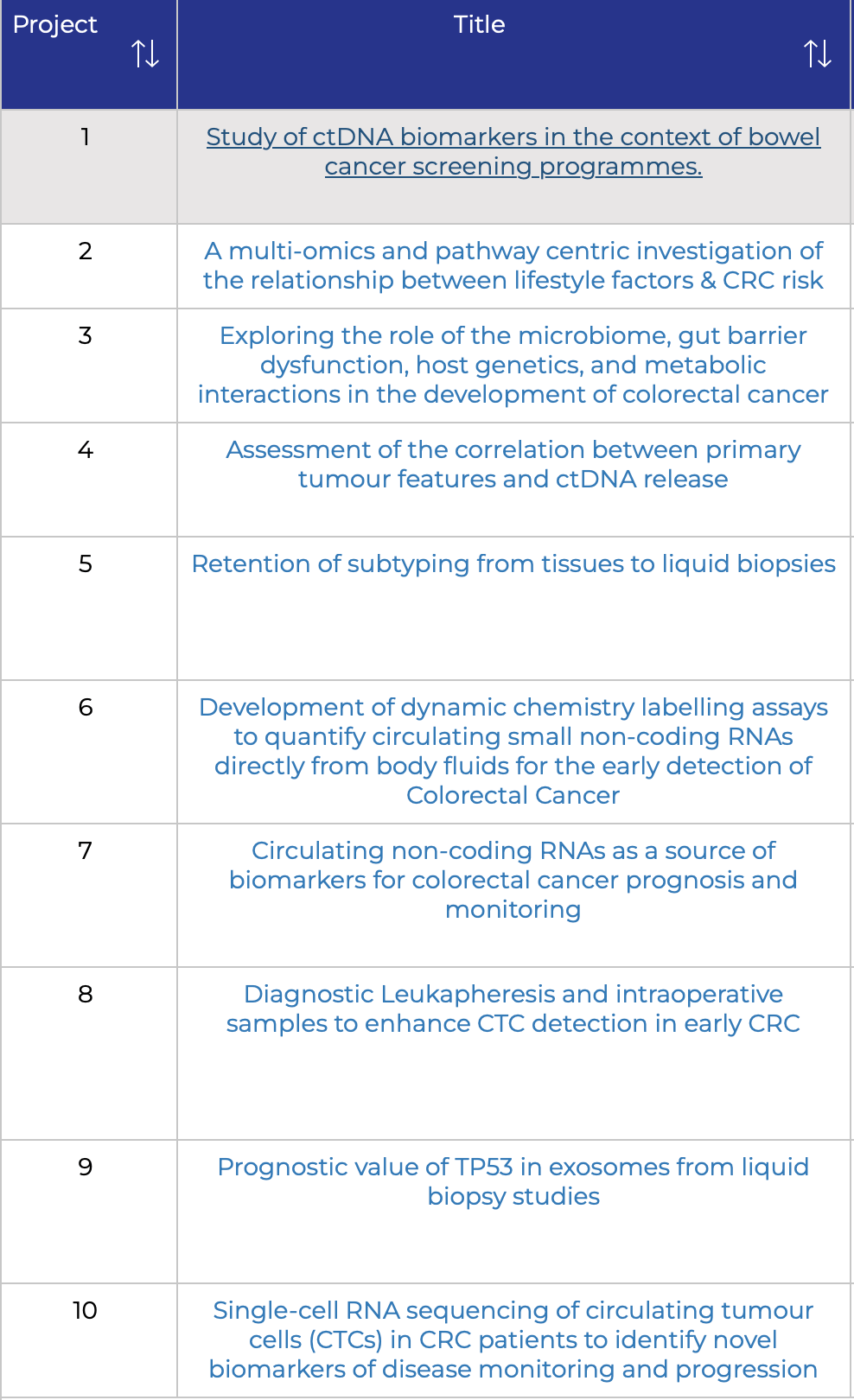
The primary scientific objective of ColoMARK will be to generate improved biomarkers for CRC by employing innovative liquid biopsy approaches. The impact of this project is paramount, as it will play a crucial role in advancing CRC prevention, treatment and management.
This project has received funding from the European Union’s Horizon Europe research and innovation programme under the Marie Sklodwska-Curie Doctoral Network Grant.
ctDNA has been widely evaluated as a novel biomarker for liquid biopsy in colorectal cancer diagnosis, prognosis and monitoring of response to treatment. Liquid biopsy based on ctDNA detection is a very sensitive test.