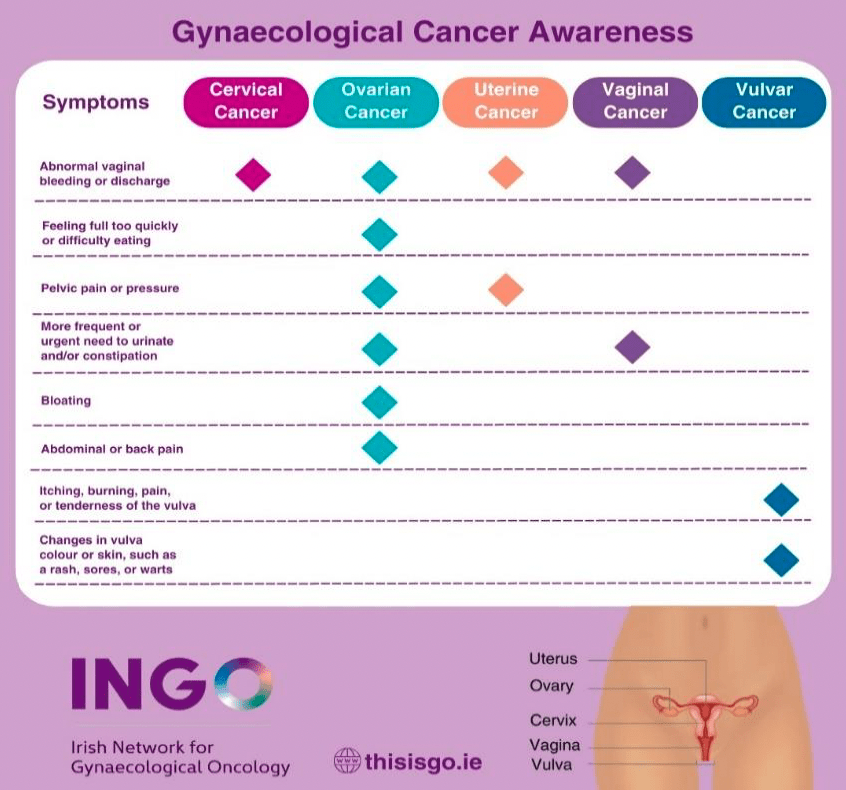
The cause of uterine (womb) cancer is unknown. But there are certain things called risk factors that can increase your chance of developing the disease. These include:
- Age: It is more common in women after the menopause between the ages of 50 and 64.
- Being overweight: If you are overweight, your risk of uterine cancer is increased.
- Hormone replacement therapy (HRT): If you are taking oestrogen-only HRT for a long time after the menopause, your risk of uterine cancer is slightly increased.
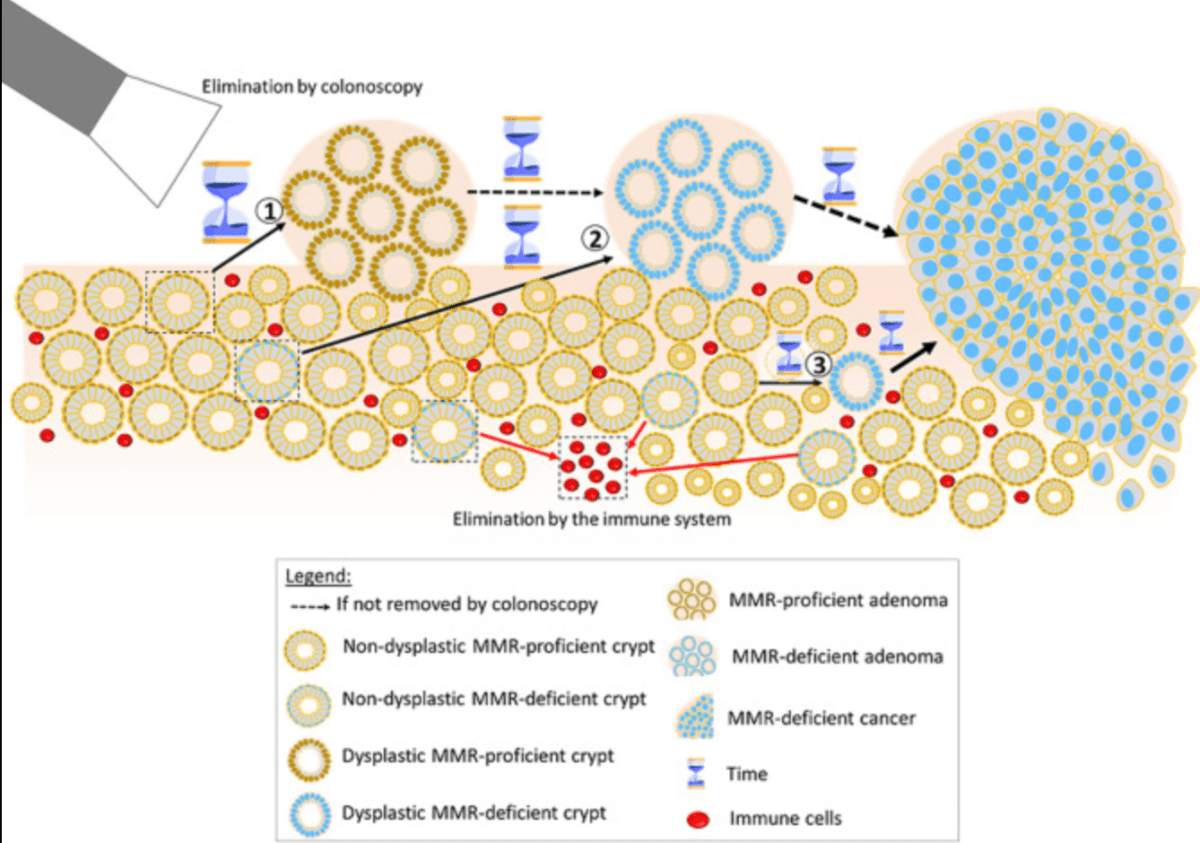
- Family history: Family history of uterine cancer in a first degree relative (mother, sister, daughter). If you have an inherited faulty gene, it raises your risk of developing uterine or bowel cancer. In a small number of families, this faulty gene can cause a condition called Lynch Syndrome .
- No pregnancies: If you have not had children or never been pregnant, your risk of uterine cancer is increased.
- Polycystic ovaries: If you have polycystic ovaries, your risk is increased. This is a condition where cysts grow in the ovaries.
- Menstrual history: If your started your periods early in life and / or started your menopause later, your risk is higher.