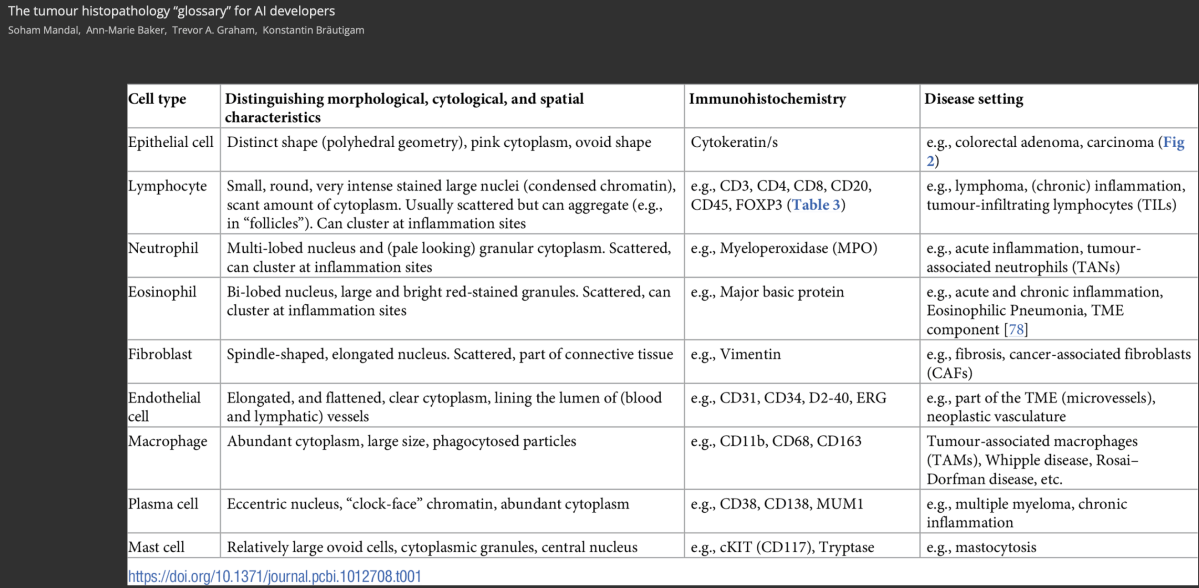
The applications of artificial intelligence (AI) and deep learning (DL) are leading to significant advances in cancer research, particularly in analysing histopathology images for prognostic and treatment-predictive insights.
However, effective translation of these computational methods requires computational researchers to have at least a basic understanding of histopathology. In this work, we aim to bridge that gap by introducing essential histopathology concepts to support AI developers in their research.
Challenges and outlook
To be implemented into routine practice, an AI algorithm needs several indispensable properties, i.e.,
clinical relevance, high accuracy, rapid implementation, fast computation, and last but not least, user-friendliness.
https://journals.plos.org/ploscompbiol/article?id=10.1371/journal.pcbi.1012708#abstract0